Both globally and in Qatar, most activities and businesses are resuming in phases, including travel and schools. While the COVID-19 pandemic has not yet been eradicated, the need for restoring normality for economic and social development is mounting. This also means that we need to learn to live with the coronavirus, albeit in a safe and measured manner. This week, QBRI experts discuss the global experience of easing lockdown restrictions and proper use of masks as a preventative measure.
Lessons Learned from the Easing of Lockdown Restrictions
The major driving force behind the relaxation of COVID-19 restrictions has been the faltering economy globally. However, reopening is like walking a tightrope: if it happens too fast, infection rates can surge, while persisting indefinitely with lockdown could cause irreparable economic damage.
Many countries who opened too quickly are now facing a rise in COVID-19 cases. Therefore, countries need to take cautious steps in a phased lifting of COVID-19 restrictions and strategies such as testing, contact tracing and lockdown management need to be strictly managed.
About 40% of all destinations worldwide have eased COVID-19 restrictions (1). Most businesses, shops and entertainment are now allowed to be open, with strict social distancing guidelines, to revive the economy and to bring back a semblance of normality to daily life. However, in countries where lockdowns were quickly lifted, such as the USA and India, this led to a huge flare-up of cases.
School reopening is central to economic revival for all countries. Most families find it difficult to return to work if schools and daycare facilities are closed. Although children do not generally suffer such severe COVID-19-related illness as adults, a cautious approach to reopening schools is nevertheless necessary.
Several countries, such as Greece, have implemented a restricted back-to-school plan with limited numbers of students per class and a combination of in-school attendance and online learning, termed ‘hybrid’ or ‘blended’ learning.
However, according to a recent UNICEF report, about a third of the world’s schoolchildren (463 million globally) do not have access to remote learning facilities (2). In such countries, the devastating effect of the disruption in education will be felt in these economies and societies for decades to come.
This virus is here to stay (3); therefore, the faster we learn to predict, track, and manage it, the better off we will be. That is why we cannot lose the “test and trace” momentum.
Since there is no single solution to tackle this pandemic, countries need to reinvent and adapt their public health system and societies. Until herd immunity is achieved or an effective vaccine is discovered, we all remain at risk. Testing, tracking, social distancing or treating infected individuals alone are not sufficient. We need a holistic approach, combining all of these tactics to combat COVID-19 (Figure 1).

Figure 1. Key lessons from global lifting of COVID-19 restrictions
Face Masks Against COVID-19
COVID-19 is primarily a respiratory disease with infection ranging from very mild, non-respiratory symptoms to severe acute respiratory illness. This infectious disease is transmitted via respiratory droplets (coughing and sneezing) or contact routes and it has been found that most of the transmission occurs from symptomatic individuals to others by not wearing appropriate personal protective equipment (PPE). Hence, it is the collective responsibility of the community to adhere to the strict guidelines put forth by the Health Ministry to prevent transmission of the disease.
Among the various PPE, masks have been recommended as an effective mode to tackle the COVID-19 pandemic. In a recent World Health Organization (WHO)-sponsored review, it was found that mask use could result in a large reduction in risk of infection (4). Moreover, a previous study on Severe Acute Respiratory Syndrome (SARS) reported that the use of masks had a strong protective impact with a risk reduction of 70% for those that always wore a mask when going out (5). Extensive research has looked into the role of facemasks in reducing COVID-19 transmission (6).
Evidence using mathematical modeling clearly shows that if most people wear a mask in public can actually prevent the spread of infection to a great extent (Figure 2) (7). A recent forecast by the Institute for Health Metrics and Evaluation (IHME) in Washington indicates a 300,000 death toll in the United States by December 2020 but this can be drastically reduced and save about 70,000 lives if 95% of the population were to wear masks. Moreover, epidemiological data from 198 countries has provided evidence that countries with strict mask mandates had lower COVID-19-related mortality (8).
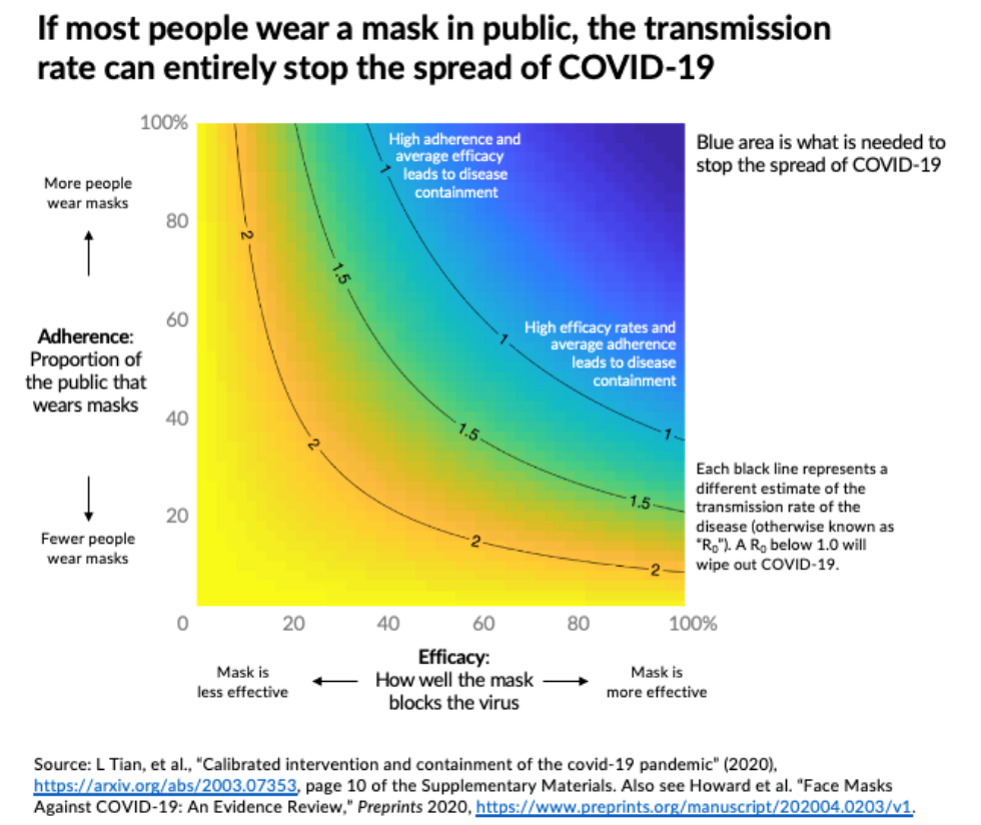
Figure 2. Simulation of COVID-19 transmission based on mask adherence and efficacy
Although the main role of masks is to protect an infected person from transmitting large infectious droplets, mask wearing as a precautionary measure is also beneficial in reducing the risk of infection. So, what are the different types of masks one can use? Based on the material used to make the mask, they can have different filtering capacities. There are basically two important considerations when looking at the efficacy of a mask: 1) the filtration of the material used and 2) the fit of the design. Recently, the WHO also published an article, “Advice on the use of masks in the context of COVID-19” (9). Based on these criteria, masks can be divided into mainly three types (Figure 3).
N95 mask
These masks are designed to ensure a close facial fit and effectively filter airborne particles. N95 masks are made of special material, which removes at least 95% of even the smallest droplets (0.3 microns). The edges of the mask are designed so that they form a tight seal around the airway (nose and mouth). These are commonly used in healthcare settings. These masks can be reused a few times unless damp or soiled.
Disposable Medical/Surgical Masks
Disposable medical masks act as a barrier between the person wearing the mask and the air around them, preventing the wearer from releasing potential contaminants into the air. They are comparatively loose fitting and the edges are not intended to form a seal around the airways. Surgical masks are made of special material that despite not forming a tight seal around the nose and mouth protects the wearer from large droplets from coughs and sneezes and prevents the wearer spreading droplets. These masks are usually one-time use and have a particle removal effectiveness of 50-75% (10).
Custom Masks
Custom masks made of cloth differ from those professionally made models. They form a much looser fit around the mouth and nose. They can also be reused after washing. They may remove some larger droplets and those captured by N95 masks. Depending on the type and material, these masks have a widely varying particle removal effectiveness of 30-90% (10).
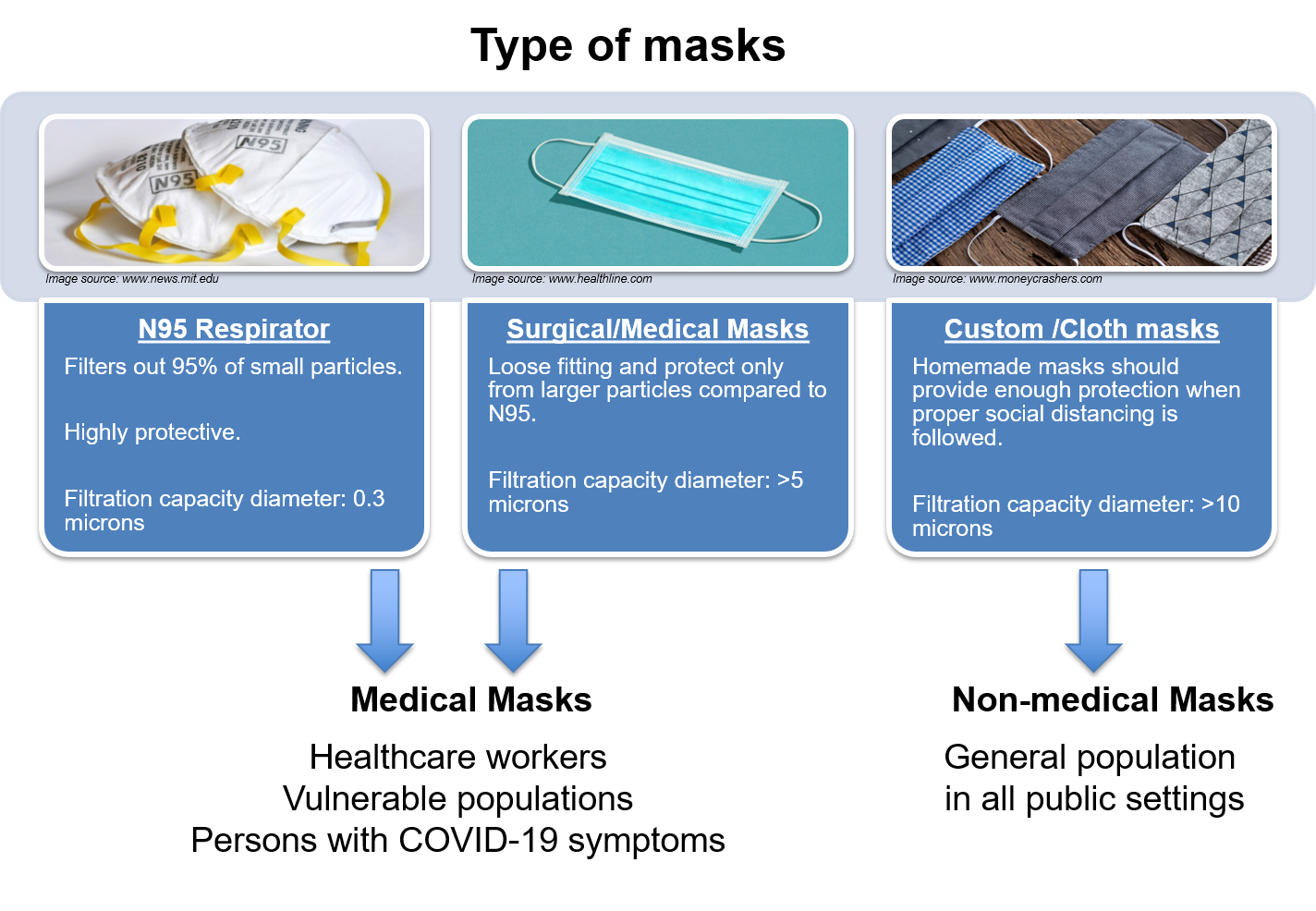
Figure 3. Types of masks
One of the main concerns about public mask wearing has not been the efficacy but how they will be used. Correct usage and management is key to ensuring the efficacy of masks (Figure 4).
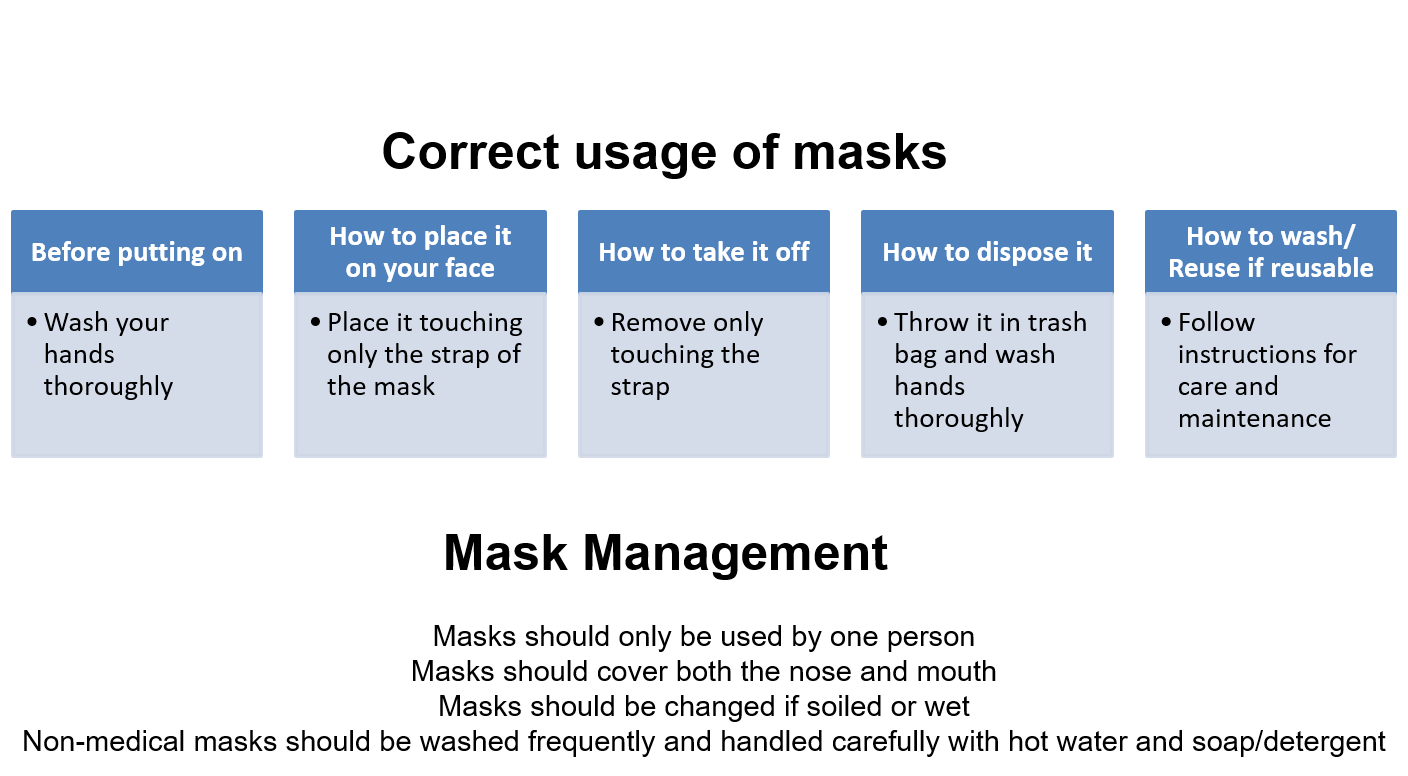
Figure 4. Mask guidelines
Due to the unprecedented pandemic caused by COVID-19, there is currently a global shortage of N95 respirators and surgical masks for use in hospitals. Several studies are now looking into the possibility of decontaminating N95 respirators with microwave- and heat-based methods, while preserving physical integrity and function.
One of the most practical solutions would be for the public to use simple cloth masks. However, the efficacy of cloth masks depends greatly on the design. Overall, it appears that cloth masks can provide good fit and filters for PPE in some community contexts but results vary depending on the material and design, the way they are used, and the setting in which they are used.
Usage of masks alone cannot be effective in stopping the spread of COVID-19. When used in combination with the strict distancing and hygiene guidelines implemented by the concerned authorities, high compliance mask mandates are a valuable tool to reduce community transmission and prevent a second wave of infections.
Section Contributors
Lessons from easing lockdown restrictions: Dr. Vijay Gupta (Postdoctoral Researcher, QBRI)
Face masks against COVID-19: Dr. Nishant N. Vaikath (Research Associate, QBRI)
Arabic text validation: Dr. Nour K. Majbour (Research Associate, QBRI)
Editors: Dr. Adviti Naik (Postdoctoral Researcher, QBRI) and Dr. Alexandra E. Butler (Principal Investigator, QBRI)
For references, please click here.
Related News