The prevalence of autism in school-age children (6 to 11 years old) in Qatar from 2015 to 2018 is estimated to be 1.14%, which means among every 87 children, there is one child diagnosed with autism [1]. Globally, April is commemorated as a month to raise awareness about autism and promote support for autistic communities. In this newsletter, Dr. Abeer Al-Shammari, a Research Fellow at Qatar Biomedical Research Institute (QBRI), part of Hamad Bin Khalifa University, gives an overview of autism and the focus of her research on the immune contexture of this disorder.
What is autism?
Autism is a neurodevelopmental disorder characterized by challenges in social interactions, speech, and non-verbal communication skills, as well as restricted and repetitive behaviors, such as hand flapping and jumping. Some medical conditions commonly co-occur with autism, such as intellectual disability, anxiety, sleep disorders, and epilepsy [2]. A child affected with autism usually displays symptoms during their first three years of life. In fact, autism is a whole spectrum of disorders, which means affected individuals exhibit symptoms at variable degrees of severity. Some individuals with autism are non-verbal while others can speak but have limited language skills; some may require significant support for performing daily routines and self-care, while others can live independently with limited support from the family or caregiver. Hence, the clinical severity of autism symptoms is largely variable among the affected individuals. There is currently no cure for autism, although early intervention and support programs, such as speech, behavior and occupational therapy, are effective in improving the outcomes in children with autism [3].
Autism risk factors - dissecting the role of the immune system
The exact cause of autism is still unclear, however genetic and environmental factors and the complex interaction between them are likely to increase the risk of developing the disorder (Figure 1). Furthermore, emerging evidence supports a link between the immune system and autism. Interestingly, genetic studies on autism revealed that several genes associated with autism are immune-related. Moreover, a majority of the environmental risk factors associated with the disorder, such as toxicants and infections, are also known to trigger immune responses [4-6].
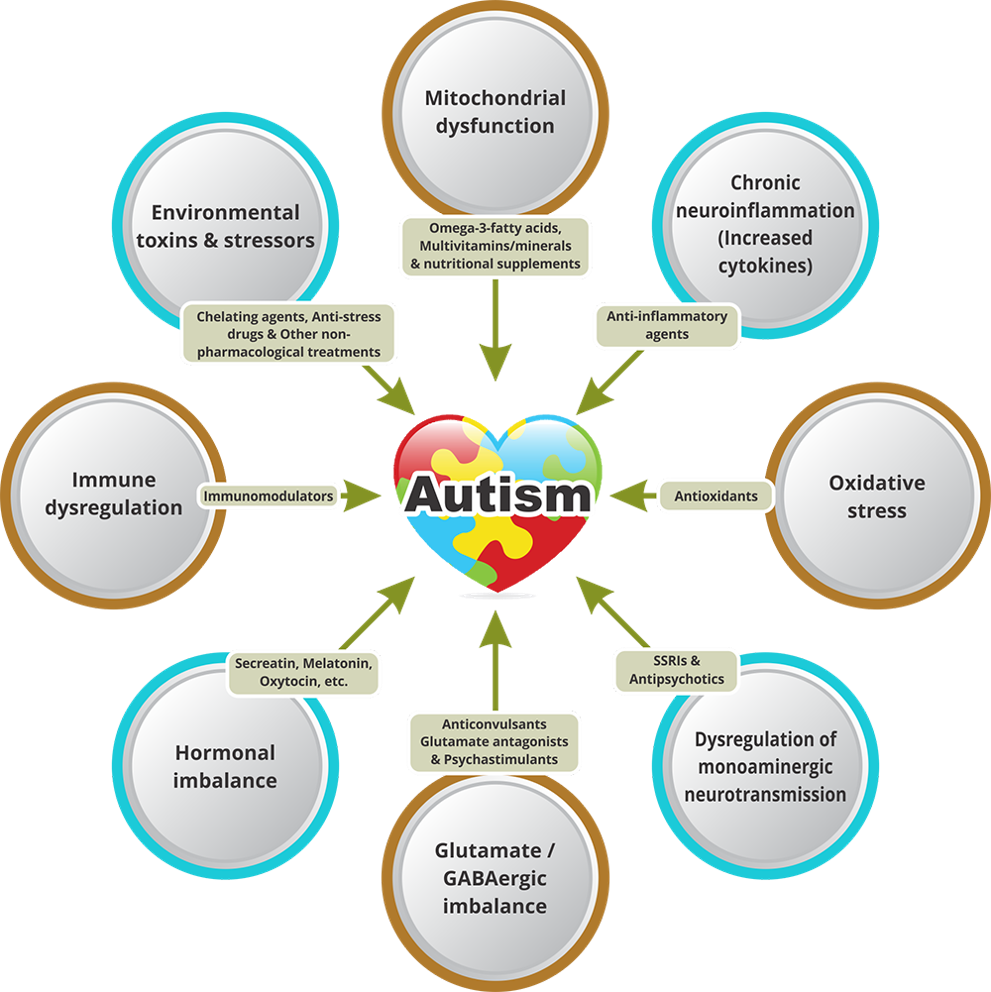
Figure 1. Risk factors associated with autism. (Source: https://www.neurogen.in/autism)
Numerous studies have reported that immune conditions, such as allergy, asthma, eczema, and gastrointestinal complications, are more common among individuals with autism in comparison to the general population [7]. These observations provide solid proof of the existence of immune dysregulation in individuals with autism and necessitate further understanding of how the immune system contributes to the risk of developing the disorder. In fact, the blood contains different types of immune cells that circulate throughout the body to mediate the function and response of the immune system. Of interest, previous studies have reported abnormalities in the circulating immune cells of individuals with autism; however, important questions remain to be addressed: What causes immune dysfunction in autism? And how do these immune alterations functionally relate to the autism disorder itself?
At QBRI, Dr. Al-Shammari’s laboratory is committed to tackling these questions, which are of significant importance towards a fundamental understanding of the autism pathophysiology (Figure 2). Her laboratory collaborates with local entities, such as the Child Development Center at Hamad Medical Corporation, for the enrollment of young children with autism, and with the Primary Health Care Corporation for the enrollment of their matching controls (children not diagnosed with autism). The enrolled participants are behaviorally assessed, and their medical history and blood samples are also collected. In Dr. Al-Shammari’s laboratory, the immune cells in the blood samples are isolated and analyzed in order to identify the specific type of immune cells being altered in the autism cohort. Further downstream, they also investigate the underlying molecular mechanisms and network interactions that potentially lead to this dysfunction, to ultimately target these factors as future potential for autism therapy. In addition, her laboratory also aims to study the translational clinical relevance of such alteration in the circulating immune cells to the phenotype and function of the brain-related cells, such as neurons and microglia, which are generated in the laboratory as cell culture models.
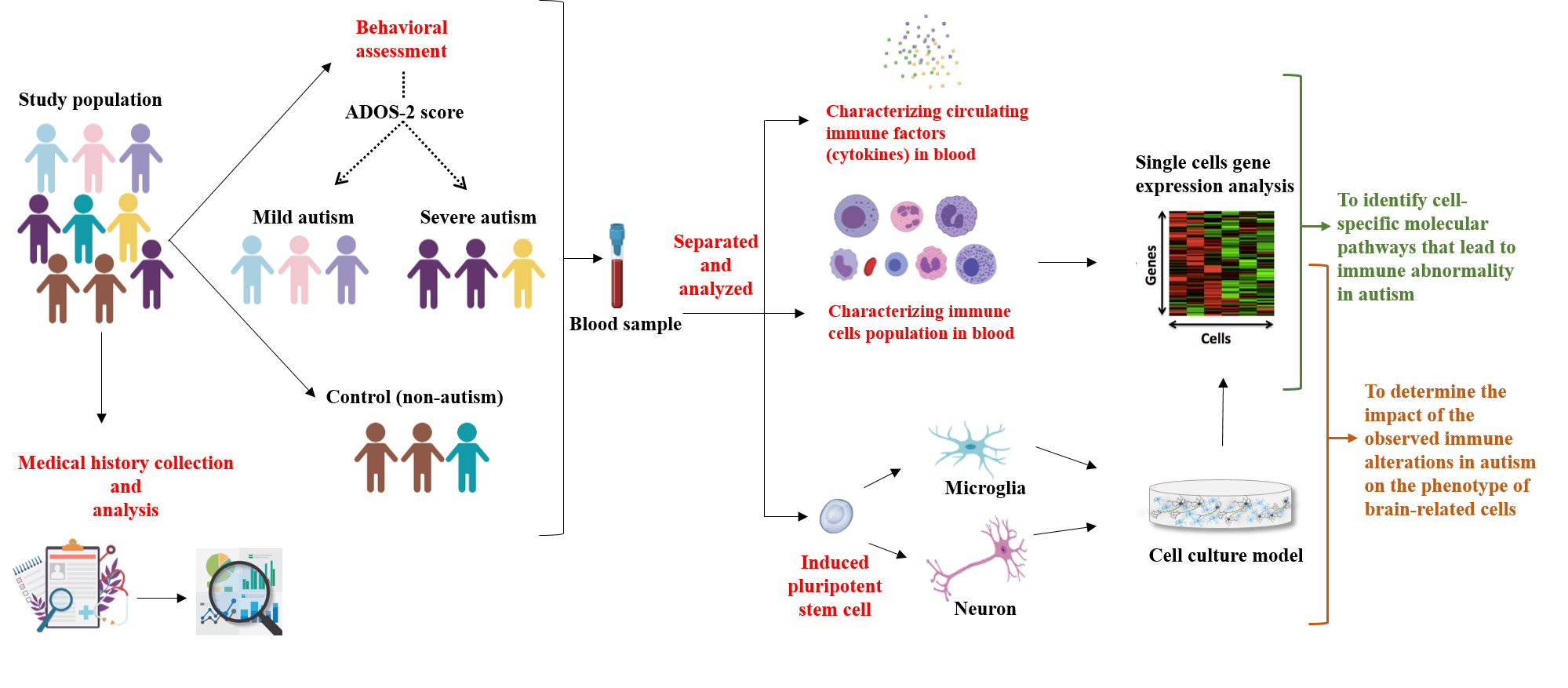
Figure 2. Schematic illustrating the research objectives at Dr. Al-Shammari’s laboratory (QBRI)
QBRI is a leading national institute with a mission to conduct translational research in selected disease areas of national priority, ultimately leading to the development of novel diagnostics and therapeutic solutions for diseases affecting the people of Qatar and the surrounding region. The research activities underway in Dr. Al-Shammari’s laboratory position her well to contribute to QBRI’s mission.
Contributed by: Dr. Abeer Al-Shammari (Research Fellow, QBRI)
Illustrations by: Dr. Wared Nour El Dine (Postdoctoral Researcher, QBRI)
Arabic text validation: Rowaida Z. Taha (Research Associate, QBRI)
Editors: Dr. Adviti Naik (Postdoctoral Researcher, QBRI), Dr. Alexandra E. Butler (Principal Investigator, QBRI)
For references, please click here.
Related News